Rubinstein-Taybi syndrome: clinical features, genetic basis
Descrição
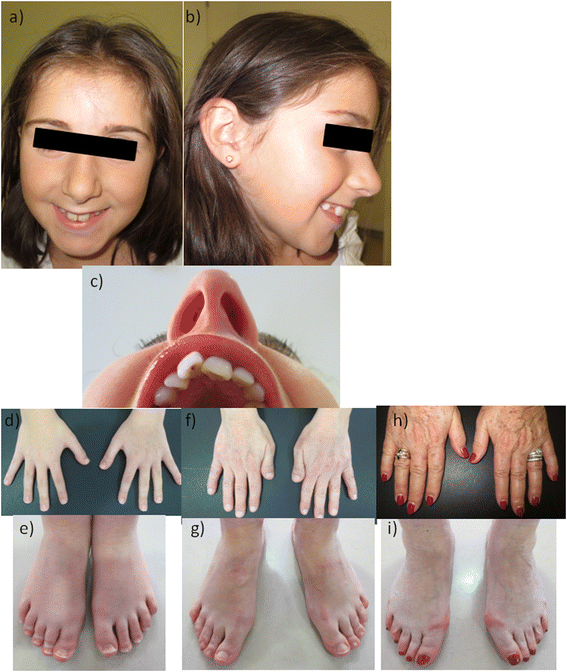
Background Rubinstein-Taybi syndrome (RSTS) is an extremely rare autosomal dominant genetic disease, with an estimated prevalence of one case per 125,000 live births. RSTS is characterized by typical facial features, microcephaly, broad thumbs and first toes, intellectual disability, and postnatal growth retardation. However, no standard diagnostic criteria are available for RSTS. In this review, we summarized the clinical features and genetic basis of RSTS and highlighted areas for future studies on an appropriate diagnostic protocol and follow-up care for RSTS. Discussion RSTS is primarily characterized by delayed growth in height and weight, microcephaly, dysmorphic facial features, and broad thumbs and big toe. Over 90% RSTS individuals with disabilities survive to adulthood, but healthcare for these patients is particularly complex, time-consuming, and costly. In addition, no standard diagnostic criteria and follow-up care guidelines are available for RSTS. It has been shown that mutations in the genes encoding the cyclic-AMP-regulated enhancer binding protein (CREBBP) and the E1A-binding protein p300 (EP300) contributed to the development of RSTS. Therefore, genetic tests are useful for the diagnosis of RSTS, although most RSTS cases are currently diagnosed based on clinical features. Summary The clinical features of RSTS have been extensively studied, which significantly contributes to the diagnosis of this extremely rare syndrome. However, the pathogenesis and genotype-phenotype associations of RSTS are largely unknown. Therefore, multicenter studies and international cooperation are highlighted for better understanding of this disease, establishing standard diagnostic criteria, and providing professional management and follow-up care of RSTS.

Rubinstein–Taybi syndrome in diverse populations - Tekendo

Cornelia de Lange Syndrome: What Is It, Causes, Signs, Symptoms
Rubinstein-Taybi syndrome with scoliosis treated with single-stage

a,b: Patient A at 3 weeks; c,d: Patient B at 6 weeks, note the
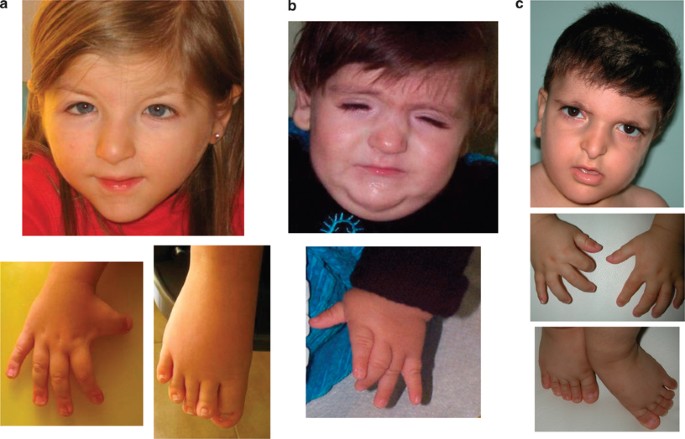
High frequency of copy number imbalances in Rubinstein–Taybi

Dysmorphic and skeletal features of Rubinstein‐Taybi syndrome
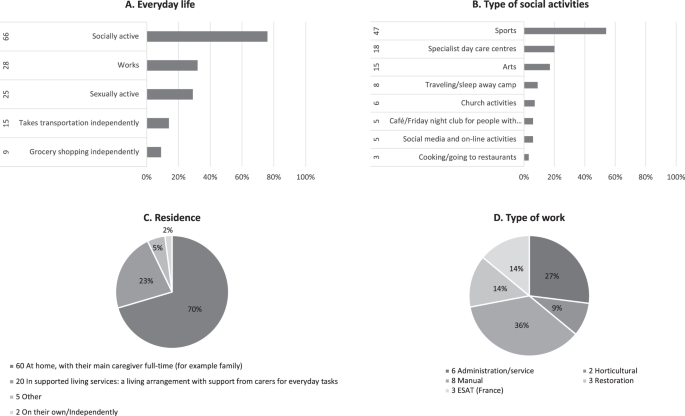
The natural history of adults with Rubinstein-Taybi syndrome: a
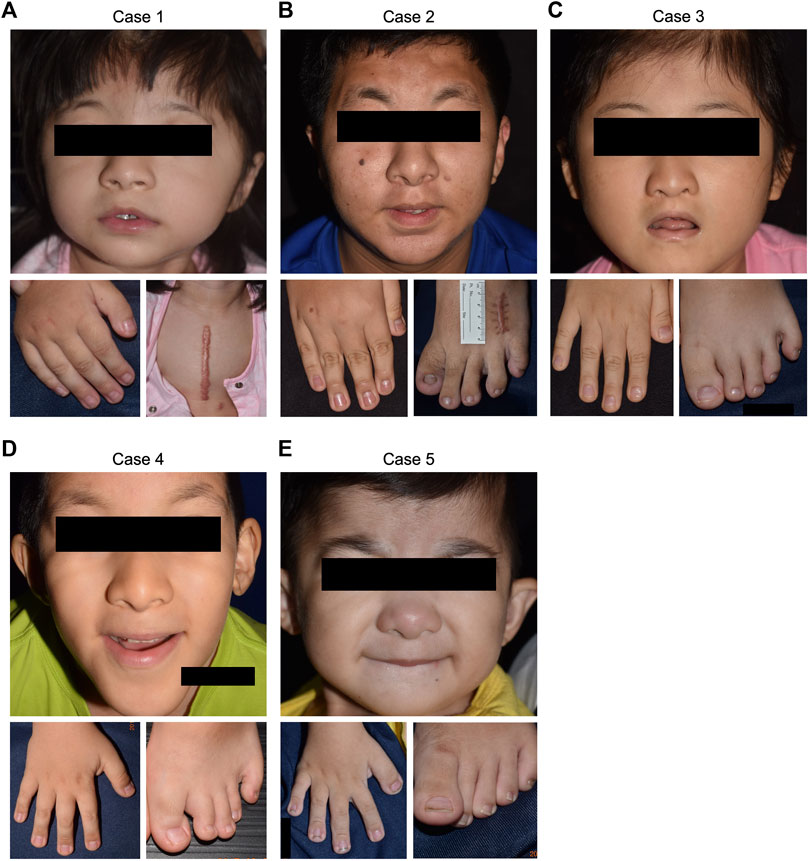
Frontiers Genetic Diagnosis of Rubinstein–Taybi Syndrome With
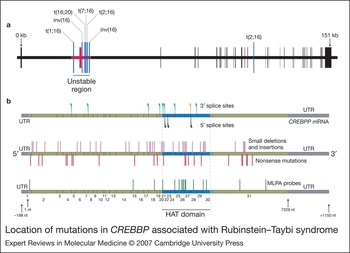
Rubinstein–Taybi syndrome: clinical and molecular overview

PDF) Oro-dental features as useful diagnostic tool in Rubinstein
de
por adulto (o preço varia de acordo com o tamanho do grupo)